St. LOUIS, Mo. (Ivanhoe Newswire) — On any given day, more than 1,600 people in North America are on a waiting list for new lungs. Many of those patients will not get the transplant they desperately need and will die on the waiting list. Doctors say one challenge is that many potential donor lungs are too damaged for transplantation. But now, new technology is reconditioning lungs and saving lives.
For 63-year-old Michele Coleman, every birthday has special meaning. Three years ago, COPD began to threaten her life.
“I collapsed in our shower. I felt like I was breathing, but I wasn’t getting any air,” Coleman told Ivanhoe.
Last year, Coleman was placed on the lung transplantation list, but a rare protein in her blood made things difficult.
“When they tell you your chances went from 100 percent to two percent of getting a donor match, it’s devastating,” Coleman detailed.
Now a new device may greatly improve the odds for patients needing lungs. It’s called the XVIVO.
“XVIVO means out of body,” said Gary Marklin, MD, Chief Medical Officer at Mid-America Transplant.
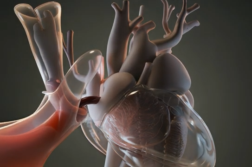
The device is a large sterile box designed to maintain and improve donated lungs. For up to six hours, lungs are placed in the machine, which brings them to body temperature. It is also a ventilator, opening up restricted airways and it circulates a special solution through the organs to improve their function.
“Its job is to take a lung that is subpar that would not be transplanted and treat it,” detailed Dr. Marklin.
Varun Puri, MD, MSCI, a cardiothoracic surgeon at Washington University School of Medicine in St. Louis said without XVIVO, only one in five donor lungs is healthy enough for transplantation. He said this device could have tremendous impact.
“My estimate is somewhere between the ten to 20 percent range increase in the number of transplants due to this technology,” detailed Dr. Puri.
Last November, Coleman received donor lungs that had been reconditioned in the box. Now the woman who couldn’t walk more than three or four steps can stroll the neighborhood with her husband.
“You’ve got to keep your hope. You cannot give up,” said Coleman.
The US Food and Drug Administration approved the device for improving lungs to use in cases with patients who have end-stage lung disease and no other options. Doctors say about half of the lungs that undergo reconditioning are eligible for transplant.
Contributors to this news report include: Cyndy McGrath, Supervising and Field Producer; Milvionne Chery, Assistant Producer; Tony D’Astoli, Editor; Brent Sucher, Videographer.
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: PHP: Lungs in a Box Save Michele
REPORT: MB #4146
BACKGROUND: Ex Vivo lung perfusion is a medical procedure used to minimize swelling in donor lungs in an effort to make them suitable enough for the transplantation. In cases for patients with end-stage lung disease, lung transplantation is often their only option for survival. However, the procedure has limited availability because not all donated lungs are safe or healthy enough to be transplanted. This unfortunate shortage of donor lungs resulted in the death of 20 percent of lung transplant candidates who were awaiting good donor lungs. Ex Vivo lung perfusion (EVLP) is a new treatment method applied to donor lungs outside of the body before the transplantation process which improves the quality of the organ, making lungs that were previously unsuited for the transplant, suited for transplant. The Ex Vivo Lung perfusion program’s ultimate goal is to expand the lung donor pool as well as extend this life-saving treatment to patients with lung disease awaiting a transplant. At the moment, EVLP is offered by a few health centers in the world and can only be accessed through a clinical trial in the United States. The overall process lasts around three-to-four hours during which the donated lungs are placed in a sterile plastic dome which is also attached to a ventilator, pump and filters. The lungs are then kept a normal body temperature and treated with a bloodless solution containing nutrients, proteins and oxygen. During the process, lung injury can be reversed and excess lung water can be removed while lung function is continuously being evaluated. Once the doctors determine the lungs suitable, this is when they are transplanted to a patient.
(Source: https://www.pennmedicine.org/for-patients-and-visitors/find-a-program-or-service/transplant-institute/lung-transplant/treatments-and-procedures/ex-vivo-lung-perfusion)
SHORTAGE OF DONOR LUNGS: According to the Thirtieth Adult Lung and Heart-Lung Transplant report in 2013 from the Registry of the International Society for Heart and Lung Transplantation, lung transplants are quite common and are being performed worldwide. The number of lung transplants being performed annually is increasing a lot. In 2011, 3,640 Lung Transplants had been performed in comparison to 1,712 annual cases a decade ago. It is a very long process for terminal stage lung disease patients before they can receive a lung transplant. Donor lungs are often subjected to many unhealthy mechanisms during the organ donation process which makes them unsuitable for sick patients therefore limiting the total number of healthy lungs. So in the end, clinical EVLP showed to have safely increased the donor pool as it preserved high-risk donor lungs with very similar outcomes to those with standard criteria donor lungs.
(Source: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4133548/ )
TECHNIQUE: The technique for the Ex Vivo Lung Perfusion assessment is very precise. First, the lungs are warmed up to a temperature of 37 degrees Celsius over a period of 20 minutes until they reach a normal state. Bronchoscopy was performed after the initiation of ventilation to clear out secretions. Blood gases were drawn from the inflow and outflow of the perfusion solution, dynamic compliance; peak inspiratory pressures, pulmonary artery pressure and pulmonary vascular resistance were assessed.
(Source: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4133548/ )
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Judy Martin
Public Relations
314-286-0105
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com