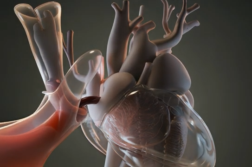
JACKSONVILLE, Fla. (Ivanhoe Newswire)— It’s a good time of year to focus on our hearts, not just because it’s Valentine’s Day, but because it’s American Heart Month. Coronary heart disease, where plaque clogs your major blood vessels, is the most common type of heart disease affecting more than 18 million Americans. Stents have become a lifesaver for the millions impacted by coronary heart disease, and now, a new stent, with a powerful name, is helping to save even the hardest to treat patients. Synergy megatron
One person dies every 36 seconds in the United States from cardiovascular disease, but this year, more than two million people will be saved by stents.
Salil Patel, MD, FACC, a cardiologist at Baptist Heart Specialists in Jacksonville, Florida says, “There are a lot of things, nowadays, that we can fix that we didn’t do before.”
Stents are a mesh tube inserted through the wrist or groin by a catheter. The tube creates a scaffold to open blockages in narrow arteries, but there are some larger vessels that previous stents could not be used in.
“Ten or 15 years ago, patients would’ve had no options. In fact, some of these patients we refer to hospice,” Dr. Patel explained.
Dr. Patel also says that a new stent, called the “Synergy Megatron”, can do what other stents can’t. The stent is built specifically for larger coronary arteries that are closer to the aorta.
“In the arteries where there’s a lot of calcium, sometimes it’s hard to expand the artery fully and get those stents to expand,” says Dr. Patel.
Made of platinum aluminum chromium alloy, the “Synergy Megatron” is stronger and can be seen more clearly on imaging, aiding doctors to place it more precisely.
Dr. Patel explains, “It can be expanded to six million meters, which is pretty large. Because we have some of this technology and newer techniques, we’re able to do some of these procedures, whereas, in the past, we wouldn’t even try it.”
Stents are permanent and should last forever. Plaque buildup can return to the area inside the stent, but that happens in just 10 percent of patients. Dr. Patel says with each new stent and technology created; the reoccurrence rate goes down.
Contributors to this news report include: Marsha Lewis, Producer; Roque Correa, Videographer, Editor.
To receive a free weekly e-mail on medical breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
Sources:
https://www.cdc.gov/heartdisease/facts.htm
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: SYNERGY MEGATRON: NEW STENT WITH MEGA SIZE, MEGA STRENGTH
AND MEGA ACCURACY
REPORT: MB #5012
BACKGROUND: A stent is a tiny wire mesh tube that props open an artery and is left there permanently. When a coronary artery, otherwise known as an artery feeding the heart muscle, is narrowed by a buildup of fatty deposits called plaque, it can reduce blood flow. If blood flow is reduced to the heart muscle, chest pain can result. If a clot forms and completely blocks the blood flow to part of the heart muscle, a heart attack results. Stents help keep coronary arteries open and reduce the chance of a heart attack. When a stent is used, it’s collapsed and put over the balloon catheter. It’s then moved into the area of the blockage. When the balloon is inflated, the stent expands, locks in place and forms a scaffold. This holds the artery open. The stent stays in the artery permanently and holds it open. This improves blood flow to the heart muscle and relieves symptoms
(Source: https://www.heart.org/-/media/files/health-topics/answers-by-heart/what-is-a-stent.pdf)
GETTING A HEART STENT: Cardiologists, vascular surgeons, and interventional radiologists all perform heart stent placements in a hospital. The procedure can take from 30 minutes to several hours, depending upon the complexity of a person’s condition. The patients will need to lie still for several hours afterward, and for larger vascular stents, they will likely stay overnight in an intensive care unit. Stent placement involves inserting a catheter into an artery, usually in the groin. The doctor feeds the catheter to the diseased artery using x-ray guidance and then injects a dye to help view the patient’s artery better on x-ray. Once the catheter reaches the blockage, a balloon or laser device opens the artery. The doctor will then place the heart stent using miniature instruments at the tip of the catheter.
NEW TECHNOLOGY: In a study, researchers at Stanford Medicine compared new stents, guided by FFR, with bypass surgery in patients who had three blocked coronary vessels. The patients, whose average age was 65, were randomly assigned to two groups, with 757 receiving the stents and 743 undergoing surgeries. In the bypass procedure, doctors took a healthy blood vessel from the patient’s leg, arm or chest and stitched it above and below the blocked artery to create a clear channel. Among the stent group, the incidence of a major complication such as death, heart attack, stroke or the need for a repeat procedure was 10.6 percent after a year. Among bypass patients, the rate was 6.9 percent, however, when the need for a repeat procedure was excluded from the equation, the figures were more aligned at 7.3 percent for stents versus 5.2 percent for bypass.
(Source: https://med.stanford.edu/news/all-news/2021/11/coronary-artery-disease-stents-bypass-surgery.html)
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Kristi Tucker
904-202-4927
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com