BALTIMORE, Md. (Ivanhoe Newswire) – Chronic pain leads to fatigue, a weakened immune system and decreased mobility – worse yet, powerful narcotics are often prescribed for patients, leading to more problems. But now, there is hope with non-invasive Scrambler therapy.
Kelly Goodwin suffers from complex regional pain syndrome, triggered by a foot biopsy five years ago.
“I couldn’t even put a sock on, the pain was so bad. The pain doctors had me on very, very high doses of, like, morphine, methadone, fentanyl, and nothing really helped,” Kelly painfully recalls.
The kind of pain she had was relentless.
Thomas Smith, MD, Professor of Palliative Medicine & Oncology at Johns Hopkins Kimmel Cancer Center explains, “You’ve got these chronic pain signals going up your spine to your brain, to the pain centers on either side, and that redistributes the blood flow. So, these areas get too active.”
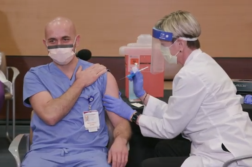
This Scrambler therapy administers stimulation through skin electrodes and scrambles pain signals.
“Do that often enough, and if you’re a person who’s responsive to Scrambler therapy, and the brain will reset and that chronic pain can go away for days, weeks or months,” Dr. Smith adds.
Each treatment takes 30 to 45 minutes per day, and it constantly shifts signals so the brain can’t get used to it. Best of all, it does not hurt.
Dr. Smith says, “To me, it feels like I’m being bitten by little tiny electric ants.”
It does it all by fooling the brain.
“For the first time, I was able to put a shoe on in five and a half years,” Kelly says.
And she has much more of an opportunity to spend precious time with her young son.
Chronic pain stems from pain impulses from damaged nerves and the failure of the inhibitory cells to block those pain signals. Dr. Smith, who just authored a study on Scrambler therapy, says it’s like a hard “reset” of the brain’s signals to eliminate the pain – like pressing “control, alt, delete” a thousand times.
Contributors to this news report include: Donna Parker, Producer; Kirk Manson, Videographer; Roque Correa, Editor.
To receive a free weekly e-mail on medical breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: SCRAMBLER THERAPY: TRCKING THE BRAIN TO FEEL LESS PAIN
REPORT: MB #5374
BACKGROUND: Chronic pain in America is a widespread and complex issue that affects millions of individuals across the country. Defined as pain that persists for weeks, months, or even years, chronic pain can significantly impair one’s quality of life, impacting their physical, emotional, and social well-being. One of the most concerning aspects of chronic pain is its prevalence. According to the National Institutes of Health, approximately 50 million adults in the United States suffer from chronic pain, making it one of the most common reasons for seeking medical care. Several factors contribute to the prevalence of chronic pain in America including underlying health conditions such as arthritis, fibromyalgia, and back problems, as well as injuries resulting from accidents or trauma. Additionally, lifestyle factors such as poor posture, lack of exercise, and obesity can exacerbate chronic pain or even contribute to its development.
(Sources: https://www.cdc.gov/mmwr/volumes/67/wr/mm6736a2.htm
DIAGNOSING: Diagnosing chronic pain is a complex process that requires a thorough evaluation of the patient’s medical history, symptoms, and physical examination. Unlike acute pain, which typically resolves with time and treatment, chronic pain persists for weeks, months, or even years, often without an obvious cause. As a result, diagnosing chronic pain requires a comprehensive approach that considers both physical and psychological factors. The first step in diagnosing is to obtain a detailed medical history from the patient including information about the onset and duration of the pain, its location and intensity, factors that worsen or alleviate the pain, any previous injuries or medical conditions, and any treatments that have been tried in the past. A family history of chronic pain or related conditions may also be relevant. Following the medical history, a physical examination is conducted to assess the patient’s overall health and identify any physical abnormalities or signs of injury. This may involve evaluating posture, range of motion, muscle strength, and sensation in the affected area. In some cases, diagnostic tests such as X-rays, MRI scans, or nerve conduction studies may be ordered to further evaluate the underlying cause of the pain.
(Sources: https://www.ncbi.nlm.nih.gov/books/NBK572296/
https://my.clevelandclinic.org/health/articles/12051-acute-vs-chronic-pain)
NEW TECHNOLOGY: New research from the University of Florida has discovered peripheral nerve stimulation. This works by delivering tiny electrical pulses to the patient’s nerves and interrupts pain messages that will decrease their pain symptoms. The doctor will implant a small wire under the skin to target individual peripheral nerves.
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Amy Mone
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com