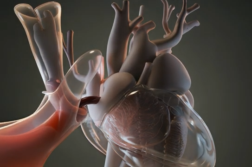
HOUSTON, Texas. (Ivanhoe Newswire) — Almost 114,000 people are on the waiting list for organ donation. On average, 20 people die every day waiting for organs to become available. Now, a new FDA-approved technology at Baylor College of Medicine, called ‘breathing lungs,’ is saving lives. The Transmedics Organ Care System keeps lungs warm by circulating blood through them, while they are transported from organ donor to recipient. Preserving the lungs.
Lung transplant recipient Cary Richardson told Ivanhoe, “You know, I smoked from an early age. I guess it was the cool thing to do, back in the day.”
Over the years, Richardson developed a very bad cough. Chronic obstructive pulmonary disorder left Richardson breathless and in need of a lung transplant.
Richardson detailed, “I had known several people and Gonzalez, who’d had lung transplants and I knew they hadn’t done very well. And, it scared me.”
Keeping lungs viable is extremely challenging.
“When an organ gets taken out of the body, travels, and then is put back into the body of another person, that’s not a natural phenomenon,” explained Gabriel Loor, MD, an associate professor of surgery at Baylor College of Medicine in Houston, Texas.
In clinical trials, ‘breathing lungs’ were used to keep the organ working. This warming approach equals more successful transplants.
Dr. Loor continued, “What this device does, is it basically takes the lung and keeps it, as if it is inside of the patient. It’s as if we’re bringing the patient directly to the recipient.”
“Once the lungs were in, I knew they were gonna be up and running,” said Richardson.
Post-surgery, Richardson used a breathing tube for only a few hours.
Richardson told Ivanhoe, “When they took it out, it was amazing. Cause when I took that first breath, it was just a sigh of relief.”
Dr. Loor said, “Our patients get so uplifted and so excited about something that’s new. Something that gives them hope.”
Dr. Loor said that in a landmark clinical trial, comparing ice to the device, it showed nearly a third of patients whose donor organs were iced down had issues. Whereas those who had the breathing lung transplant experienced far more successful outcomes.
Contributors to this news report include: Cyndy McGrath, Executive Producer; Donna Parker, Field Producer; Bruce Maniscalo, Videographer; Roque Correa, Editor.
To receive a free weekly e-mail on Medical Breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: PRESERVING LUNGS OUTSIDE THE BODY!
REPORT: MB #4720
BACKGROUND: There are nearly 2,000 people who receive a lung transplant each year in the U.S. There are four types of transplants that doctors perform: single lung, double lung, bilateral sequential, which is a double lung surgery at the same time and a heart-lung transplant which comes when the heart and lungs are from the same donor. Pulmonary hypertension, heart disease, pulmonary fibrosis and chronic obstructive pulmonary disease are all conditions that could lead to a lung transplant, but they do not require a transplant. For those with lung cancer, healthcare providers do not advise a lung transplant.
(Source: https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/lung-transplant https://www.uofmhealth.org/conditions-treatments/transplant/adult-lung-transplant)
PREPARING: Doctors may conduct numerous tests, like a chest x-ray, CT scan, pulmonary function test, coronary artery catheterization, and cardiac stress test. If patients have significant heart, liver or kidney disease, cancer, ongoing infections or are continually smoking, they will not receive a lung transplant. Patients are placed on the list based on their lung allocation score, which tries to predict how long a patient is likely to live without a lung transplant and how long they may live after receiving the transplant. Higher scores are considered first when lungs are available. Those who receive a transplant will need to go on a cardiopulmonary bypass during the surgery, which means the blood is pumped and enriched with oxygen by a machine rather than by the heart and lungs.
(Source: https://www.webmd.com/lung/lung-transplant-surgery#3)
NEW PROCEDURE: The first breathing lung transplants occurred in 2012 by UCLA Health. Normally, lungs are transplanted through ambulance, helicopter or airplane. The lungs are removed and placed in three sterile bags on ice which is kept between 0 and 4 degrees. But they do not always make it; some of the lungs may have deteriorated since the tests were performed as there is only a six-hour window. The Organ Care System eliminates that window and can even improve the lungs that are in transit because of the temperature they are held at. They want to take this procedure and move it to heart donors as well.
(Source: https://www.uclahealth.org/transplants/lung/breathing-lung-transplant https://utswmed.org/medblog/lung-transplant-journey/)
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Dipali Pathak, Assistant Director of Communications
Baylor College of Medicine
713-798-6826
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com