CLEVELAND, Ohio (Ivanhoe Newswire) — Cancer, COPD, fibrosis, there are many reasons why someone may need a lung transplant. But thousands of people waiting will never get one in time. In fact, 80 percent of the lungs that are donated for possible transplants are discarded due to poor function or disease. But now, a new innovative procedure can restore compromised, donated lungs, and help save more lives.
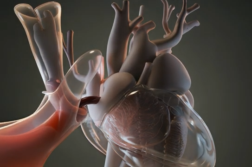
This is a donated lung being restored to almost new to save the life of this man, Dan Lynch.
Every breath was a struggle for this grandfather of seven.
“It’s not a very promising prognosis,” Dan shared with Ivanhoe.
Dan was suffering from idiopathic pulmonary fibrosis, a disabling lung disease with no known cure.
Kenneth McCurry, MD, cardiothoracic surgeon at the Cleveland Clinic explained, “He was very sick by the time he came to a transplant.”
With few options and no viable transplant, surgeons at the Cleveland Clinic used ex vivo lung perfusion, or EVLP, to restore a not-so-perfect, donated lung for Dan. The donated lung was attached to a miniature heart-lung machine. For the next six hours, fluid and oxygen pumped through the organ. This process removes excess water and reverses some existing injuries that would otherwise have kept it from meeting transplant requirements.
“We were quite amazed that there were some lungs that we perfused that we didn’t think would be usable, but they got much better on the machine and performed quite well when we ended up transplanting them in a patient,” Dr. McCurry recalled.
Forty-five patients, including Dan, received transplanted lungs they wouldn’t have without EVLP.
“So that’s 45 patients that otherwise may have not gotten a lung or a set of lungs and may have died waiting for a set of lungs,” clarified Dr. McCurry
Lynch shared, “I feel good. I feel great, and I’m very grateful.”
Ready to return to grandpa duty.
There’s no additional risk to the patient receiving a perfused lung and rejection rates have not increased. In 2017, the most recent year where numbers were available, 1,300 people were on the waiting list for lungs. More than 300 died waiting for a suitable organ. Livers and kidneys are also being perfused and Dr. McCurry hopes to begin perfusing intestines and other organs in the future.
Contributors to this news report include: Cyndy McGrath, Executive Producer; Marsha Lewis, Field Producer; Kirk Manson, Videographer; Roque Correa, Editor
To receive a free weekly e-mail on Medical Breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: NEW AND IMPROVED DONATED LUNGS
REPORT: MB #4756
BACKGROUND: A lung transplant surgery occurs when a diseased lung needs to be replaced with a healthy lung from another person. Transplant becomes a viable option when a patient has a serious complication like cystic fibrosis, COPD, or pulmonary fibrosis that cannot be treated in any other way and the patient has a life expectancy of 12 to 24 months without a transplant. This procedure is done on patients of all ages ranging from infants to seniors. There are multiple types of lung transplant procedures such as single and double lung, taking out one or both lungs respectively. Bilateral sequential or bilateral single, meaning removing both lungs at the same time and heart-lung transplant which involves transplanting both lungs and the heart from one person to another. Most commonly, lungs are transplanted from deceased organ donors. However, it is also possible for healthy, living individuals to transplant a portion of their lung, or a lobe, to another person and still live a normal life with the remaining lung.
(Source: https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/lung-transplant)
TRANSPLANT LIST: A new name is added to the transplant list every ten minutes. On average, 20 people die every day waiting for a new organ and there are currently 1,189 people on the waiting list for lungs in the United States. For example, only 42 percent of cystic fibrosis patients received donated lungs viable for transplant between 2003 and 2006 and there were still 1,079 patients waiting. Often, even when donor lungs become available, they are not usable enough to warrant a successful transplant. Due to this discrepancy, thousands of people can’t get the lifesaving organs they need. In 2011 through 2014, after waiting a year, with 1,216 people still remaining on the list, only 63.7 percent of patients received a lung transplant. In 2016, 221 lungs were deemed “unsuitable” for transplant due to “disease, injury to the organ, and the lapse of too much time between recovery and transplantation,” according to a 2017 report from the National Academies of Sciences, Engineering, and Medicine.
(Source: https://www.americantransplantfoundation.org/about-transplant/facts-and-myths/, https://optn.transplant.hrsa.gov/data/view-data-reports/national-data/#, https://www.nap.edu/read/24884/chapter/3#36, https://www.tmc.edu/news/2019/06/bioengineered-lungs-how-long-from-pigs-to-people/)
NEW TECHNOLOGY: A new technique, called ex vivo lung perfusion, or EVLP, aims to expand the availability of suitable donor lungs and shorten patient wait times. In the United States alone, 1,600-1,800 lung transplants are performed each year, with many patients dying prior to organs becoming available for them. And, nearly 80 percent of lungs cannot be used. Traditionally, organs have been put in cold storage after procurement where a lot of damage and degradation can occur. By performing ex vivo lung perfusion, the lungs are kept alive outside the body with high oxygen and fluids flowing through them. This prevents the damage and degradation caused by cold storage. The Cleveland Clinic initiated EVLP research activity in 2011 in the McCurry lab and investigated 50 rejected donor lungs. Ex vivo lung perfusion is meeting the high demand for utilizing as high of a percentage as possible of one of the rarest and most desired organs on the transplant list.
(Source: https://consultqd.clevelandclinic.org/increasing-transplantable-donor-lungs-ex-vivo-lung-perfusion/, https://www.upmc.com/services/transplant/lung/process/surgery/ex-vivo-lung-perfusion)
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
ANDREA PACETTI, PUBLIC RELATIONS
CLEVELAND CLINIC
(216) 316-3040
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com