CLEVELAND, Ohio (Ivanhoe Newswire) – A rare autoimmune condition was slowly choking the life out of a 40-year-old mother of four. After months of unsuccessful treatments, doctors used a little-known procedure to restore her lungs to normal called lung washing.
The Crider family was wrapping up an active Disney vacation in March of 2019 when Paula Crider could no longer ignore her extreme shortness of breath.
“The day before we left to come back home, Kaitlyn said to me, ‘Mom, your lips are blue’,” Crider recalls.
A nurse checked her blood oxygen level. Normal is a high of 90. Crider’s reading was 76. Ultimately, she was hospitalized and diagnosed with a very rare autoimmune condition.
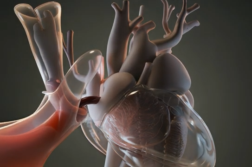
Crider was diagnosed with PAP, which stands for pulmonary alveolar proteinosis. PAP is a condition that causes protein-filled fluid to block the lungs, slowly suffocating the patient.
Crider says, “Their first thought was that I had to have a double lung transplant because I was so bad, and I just kept getting worse.”
Instead, doctors at the Cleveland Clinic used a procedure called whole lung lavage, also known as lung “washing.” During the procedure, doctors attach one lung to a ventilator, then they pump a saline solution into the other lung.
“They keep doing that liter, and liter, and liter, and liter, and liter, and liter until the fluid coming out is the same color as the fluid going in, which is to say clear,” Leslie Tolle, MD, pulmonologist at the Cleveland Clinic, explains.
Crider was determined to fight the PAP without missing a beat. In fact, she completed her master’s degree during a month-long hospital stay, graduating with a perfect 4.0.
“I am oxygen free, for right now. It’s been amazing,” Crider expresses.
PAP is considered an “orphan,” or extremely rare disease, affecting one in 100 thousand people worldwide. It’s estimated that 10,000 people in the United States have the rare disease.
Contributors to this news report include: Cyndy McGrath, Producer; Kirk Manson, Videographer; Roque Correa, Editor.
To receive a free weekly e-mail on medical breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
Source:
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: LUNG WASHING SAVES PAULA’S LIFE
REPORT: MB #5088
BACKGROUND: Pulmonary alveolar proteinosis, or PAP, is a syndrome, a set of symptoms and signs – not a single disease, in which surfactant in alveoli builds up slowly. This blocks air from entering alveoli and oxygen from passing through into the blood, which results in a feeling of breathlessness. Autoimmune PAP occurs in six to seven people per million individuals in the general population. It most commonly presents in adults of 30 to 40 years of age but can occur in children as young as three years old. It is more common in men, presumably because more men smoke.
https://rarediseases.org/rare-diseases/pulmonary-alveolar-proteinosis/)
DIAGNOSING: In most PAP cases in adults, the cause is suspected to be a lack of or a problem with granulocyte-macrophage colony-stimulating factor (GM-CSF). This substance is needed to make certain immune cells develop. Without it, the air sacs are not able to clear out all traces of protein-containing materials. This leads to accumulation of debris in the air sacs and eventually to breathing problems. PAP has symptoms like shortness of breath, which is called dyspnea, chest pain or tightness, fever, weight loss, sometimes a cough, low levels of oxygen in the blood, and abnormal growth of toenails or fingernails.
(Source: https://my.clevelandclinic.org/health/diseases/17398-pulmonary-alveolar-proteinosis-pap)
NEW TECHNOLOGY: Faced with the global need for affordable, safe, easy-to-use and easy-to-maintain respiratory support technology, the researchers in the NeoRest team have invented a device that can provide critical respiratory support to infants who may otherwise receive little or no assistance. The device, called Seattle Children’s Positive Airway Pressure (Seattle-PAP) device, is similar to, but fundamentally improves upon, a commonly used respiratory support technology called Bubble Continuous Positive Airway Pressure (B-CPAP). The team’s Seattle-PAP device improves upon conventional B-CPAP by providing an equivalent mean airway pressure accompanied by oscillations that may reduce the likelihood an infant will need to receive mechanical ventilation. The key difference of the Seattle-PAP device is that the expiratory tube is placed in the water at a 135° angle; conventional B-CPAP tubes are placed in the water at 0° (straight down). It is this change in angle that more consistently produces the range of oscillations thought to improve lung function and make it easier for an infant to breathe.
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Alana Wyche
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com