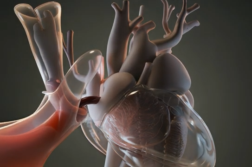
CHICAGO, Ill. (Ivanhoe Newswire) – More than 2,500 people received new lungs last year. Cystic fibrosis, COPD, breathing disorders, and heart disease are some of the main reasons. But did you know lung transplants for lung cancer are extremely rare? A double lung transplant on a terminal lung cancer patient is even more rare. But, by doing it on one man, doctors may save many more.
Fifty-four-year-old Albert Khoury was losing his battle to stage four lung cancer. Khoury ended up in the ICU with pneumonia and sepsis. He was fading fast, yet his cancer remained contained to his lungs.
“We saw that his cancer cells did not spread outside the lung. It kept spreading inside the lung to the opposite part of the lung. So, he wasn’t able to breathe,” Northwestern Medicine oncologist, Dr. Young Chae, MD, explains.
That’s when the team at Northwestern decided to give Khoury an extremely rare double lung transplant.
Thoracic surgeon at Northwestern Medicine, Dr. Ankit Bharat, MD, says, “You can imagine trillions and trillions of these cancer cells all over both his lungs. We had to, very meticulously, take all of that out within that six- hour time constraint that we typically have for reimplantation of new lungs.”
Six months later after his transplant, there was no trace of the cancer coming back.
Dr. Chae expresses, “Just to see a new lung, clean lung, is surreal.”
This one man’s story, now giving hope to others who may have lost theirs.
“This message is for everybody who has cancer. Just stay strong. Fight. Don’t stop. Good things will happen,” Khoury exclaims.
Albert Khoury was and is a non-smoker. He’s not alone. Up to 20 percent of the people diagnosed with lung cancer have never smoked. Doctors at Northwestern tell us although Albert was the first lung cancer patient to receive new lungs, he won’t be the last. They are starting a registry to keep track of similar patients treated at Northwestern.
Contributors to this news report include: Marsha Lewis, Producer; Roque Correa, Videographer & Editor.
To receive a free weekly e-mail on medical breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
Sources:
https://www.thoracic.org/patients/lung-disease-week/2022/lung-transplant-week/
https://www.cancer.gov/news-events/press-releases/2021/lung-cancer-never-smokers
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: LIFESAVING DOUBLE LUNG TRANSPLANT
REPORT: MB #5132
BACKGROUND: A lung transplant is a surgical procedure to replace a failed lung with a working one. They usually come from a deceased donor. Lung transplants are prearranged for people who have tried medications and treatments but have failed to improve lung function. More than 25,000 lung transplants were made last year. A transplant can replace one or both lungs. The surgery is a major operation with high risks, but in the end drastically helps your quality of life. It is often used in patient cases of: Chronic obstructive pulmonary disease, cystic fibrosis, and high blood pressure in the lungs.
(Source: https://www.mayoclinic.org/tests-procedures/lung-transplant/about/pac-20384754)
DIAGNOSING: Many damaged lungs can be treated with medications and breathing devices. When these operations fail to help doctors will often recommend a lung transplant. Transplants require waitlist and can often take a very long time to qualify for. Lung transplants are not the best option for all cases. All cases are considered from transplant centers, however, active infection, sever liver and heart disease, and recent history of cancer are often not considered appropriate for a transplant.
(Source: https://www.mayoclinic.org/tests-procedures/lung-transplant/about/pac-20384754
NEW TECHNOLOGY: Lung transplants for cancer are very rare. Subtypes of lung cancer in non-smokers are found to have distinct evolutionary characteristics and molecular processes. This has caused a future of different treatments for the subtypes. A study by international team led by researchers at the National Cancer Institute used a large epidemiological study of genome sequencing to evaluate changes in tumor tissue and normal tissue from 232 nonsmokers. The study allowed researchers to see subtypes distinguished and different approaches to be taken. A better understanding of how tumors evolve and the way lung transplants can contribute to these subtypes are being examined in new research.
(Source:
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Megan McCann
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com