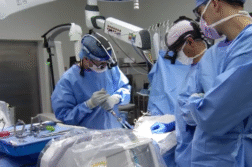
MIAMI, Fla. (Ivanhoe Newswire) – More than a million and a half people in the U.S. undergo back surgery each year, however, classic back surgery has one of the highest failure rates of any surgery – they call it “Failed Back Surgery Syndrome” and it means patients get no relief from their pain after back surgery. But now, some people are opting for a second revision surgery for help.
Knead it. Toss it. Pile on the toppings, and bake! Chef Renato Viola has been doing this since he was a kid – a champion dough thrower, he now runs 13 pizza shops across the country – he says he can’t remember a time when his back didn’t hurt.
Renato tells Ivanhoe, “Pain was part of my life. Tossing the pizza was not easy.”
Renato tried everything to relieve the pain from a herniated disc — surgery was a last resort. But Renato is one of up to 40 percent of patients whose back surgery didn’t help. Orthopedic spine surgeon, Georgiy Brusovanik, MD specializes in revision back surgery.
“This disc does not look normal. In fact, there is a large part of that disc that’s sitting in the canal, and there, you can see a nerve that’s being compressed by that disc,” Dr. Brusovanik describes.
This was what was causing Renato’s pain.
Dr. Brusovanik says, “The pain was constant. He couldn’t sleep, he couldn’t lay down, he couldn’t sit, he couldn’t walk.”
Dr. Brusovanik performed a minimally-invasive micro discectomy.
“Where you sneak in carefully, protect the nerve and remove the little piece of disc that has exited the disc proper into the canal,” he adds.
The second time was a success. After revision surgery, Renato is back in the kitchen — this time, pain-free. Dr. Brusovanik says there are three things patients suffering from back pain should ask their doctors: first, why are you suffering? Being old is not a good answer. The second question, do you have experience dealing with this type of problem and ask to talk to a former patient, and if the doctor is blaming you for the failed procedure, it might be best to find a new surgeon.
Contributors to this news report include: Marsha Lewis, Producer; Matt Goldschmidt, Videographer; Roque Correa, Editor.
To receive a free weekly e-mail on medical breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
Source:
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TITLE: RELIEVING BACK PAIN: FIXING FAILED SPINE SURGERIES
REPORT: MB #5372
BACKGROUND: Failed Back Surgery Syndrome (FBSS), also known as Failed Back Syndrome (FBS), refers to a condition where patients continue to experience persistent pain or other symptoms following one or more spine surgeries. It’s a complex and challenging condition that can significantly impact a patient’s quality of life. Failed Back Surgery Syndrome affects 10 to 40% of patients who undergo back surgery. FBSS can have various causes, including inadequate surgical decompression, incomplete resolution of the underlying spinal pathology, nerve damage during surgery, scar tissue formation, infection, hardware failure, adjacent segment degeneration, or psychological factors such as depression and anxiety.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5388346/)
DIAGNOSING: The symptoms of FBSS can vary widely depending on the underlying cause and the specific structures affected. Common symptoms include, but are not limited to: new pain at a level different from treated location, persistent or recurrent back pain, numbness or tingling sensations, muscle weakness, restricted mobility, back spasms, and/or potential dependence on pain medication. Diagnosis of FBSS involves a comprehensive evaluation of the patient’s medical history, including previous surgeries, imaging studies such as X-rays, MRI, or CT scans to assess the spinal anatomy, and physical examination to evaluate neurological function and musculoskeletal integrity.
(Sources: https://weillcornell.org/failed-back-surgery-syndrome
NEW TECHNOLOGY: The newest treatment for failed back surgery syndrome is called a minimally-invasive discectomy. Orthopedic spine surgeon, Georgiy Brusonavik, MD, specializes in this procedure. “A minimally invasive discectomy is a procedure where a spine surgeon sneaks into the spine with a patient who has a disc herniation, removes the part of the disc that snuck out and then sneaks out of the spine without hurting anything. Essentially, the approach maximizes visualization by using specialized tools and specialized light and microscope, but minimizes the risk of injuring musculature. Patients usually return to their work within about a week or two. They rarely need physical therapy, brace or any kind of restrictions.”
(Source: https://spinedoctormiami.com/patient-education/minimally-invasive-discectomy/)
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Joanna Palmer
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com