CLEVELAND, OH (Ivanhoe Newswire) CTEPH is high blood pressure in the lungs caused by blood clots. Doctors say it is an under recognized, under diagnosed disease, causing fatigue, trouble breathing, lightheadedness, and passing out. At one time, the only effective treatment was surgery, but that’s not an option for 40 percent of patients.
Peggy Notman lived a busy life. But then her lungs started keeping her out of work and in the house.
“I was walking my dog and I was totally out of breath,” said Notman.
When her first grandchild was born, Notman knew something had to change.
“I want to see that baby grow up and be able to see every grandchild that comes along. And I want them to know me. Not just know me by pictures,” Notman shared.
After years of misdiagnosis, doctors discovered Notman had CTEPH.
“Chronic thromboembolic pulmonary hypertension is high blood pressure in the lungs due to chronic blocked lungs,” explained Gustavo Heresi, MD, Director of the Pulmonary Vascular and CTEPH Program at Cleveland Clinic.
But she was not a candidate for traditional treatments. That’s when doctors from the Cleveland Clinic told her about balloon pulmonary angioplasty or BPA.
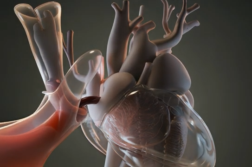
“And we’re able to go in there with catheters, wires and balloons and with x-ray and ultrasound guidance we’re able to get in, find the webs that are associated with chronic pulmonary hypertension from chronic PEs and basically open them up to optimize the blood flow,” said Ihab Haddadin, MD, an Interventional Radiologist at Cleveland Clinic.
Notman needed repeat procedures. She noticed a difference after the second procedure. And by the sixth one …
“Now I can go out and do things that I need to do, that I want to do and feel confident that I’m not going to pass out,” Notman said.
The ideal candidate for BPA is a CTEPH patient who has clots that are too small and are beyond the reach of surgical instruments. Dr. Haddadin says the benefits increase with multiple procedures. Risks include getting excess fluids in the lungs and hemorrhage, but so far Dr. Haddadin says he is happy with the results.
Contributors to this news report include: Cyndy McGrath, Supervising Producer; Hayley Hudson, Assistant Producer; Roque Correa, Videographer; Robert Walko, Editor.
To receive a free weekly e-mail on Medical Breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: BPA: BETTER BREATHING FOR LUNG PATIENTS
REPORT: MB #4499
BACKGROUND: Chronic thromboembolic pulmonary hypertension (CTEPH) can develop in people who have experienced an acute pulmonary embolism (a blood clot in your lungs [PE]). In fact, as many as one out of every 25 people who had a PE, even those who were treated with at least 3 months of blood thinners, could develop CTEPH. While CTEPH is rare, it generally appears in someone within six months to two years of experiencing an acute PE. Unfortunately, there is no way for a doctor to tell that you have CTEPH based on symptoms alone. This is because the most common symptoms of CTEPH are also common symptoms of other diseases, such as asthma, chronic obstructive pulmonary disease (COPD), heart failure, or acute PE.
(Source: https://www.cteph.com/basics/symptoms-and-risk/)
TREATMENT: The definitive treatment for CTEPH is a delicate surgery called a pulmonary thromboendarterectomy (PTE), also referred to as a pulmonary endarterectomy. This surgery is done while the heart is stopped, and a heart-lung bypass machine does the work of the heart and the lungs. The surgeon carefully removes the clots from the pulmonary arteries. PTE surgery is curative in over 90 percent of patients. For patients who are not good candidates for PTE, either due to chronic clots that are not easily accessible to the surgeon or who have other medical conditions which make PTE too risky, there are other options. A newer procedure called balloon pulmonary angioplasty uses a tiny balloon which is inflated inside the pulmonary artery to reduce the narrowing and open the vessel.
NEW TECHNOLOGY: Researchers collected and analyzed data from 308 patients who underwent 1,408 procedures at seven institutions in Japan. Blood pressure and blood flow were found to have improved significantly in 249 patients who underwent BPA. Improvements of blood flow were maintained in 196 patients who underwent right heart catheterization during the follow-up period. The need for oxygen supplementation and PH-targeted therapies also decreased. The researchers note that overall survival rates after BPA are similar to the standard PEA treatment. Overall survival after the initial BPA procedure was 96.8 percent at one and two years. At three years, it was 94.5 percent.
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Andrea Pacetti, Senior Manager, Public & Media Relations
216-444-8168
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com