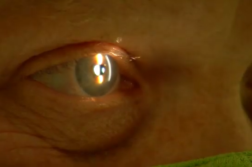
CHAPEL HILL, N.C. (Ivanhoe Newswire) – It’s something we all do, and never even realize we are doing it – blinking. But up to 10,000 people a year lose their ability to blink, and that can cause serious problems — even causing people to go blind. Now, a new technique is saving sight, even reversing vision loss.
Most people blink 17 times a minute – over a thousand blinks every hour – that adds up to 15,000 blinks a day, but some people can lose their ability to blink.
“N.K. stands for neurotrophic keratopathy, or neurotrophic keratitis, and it describes a condition in which the nerves that provide sensation to the surface of the eye, and specifically the cornea, are damaged in some way and not working properly,” explains Ophthalmologist & Oculofacial Plastic Surgeon at UNC School of Medicine in Chapel Hill, N.C, Daniel Rubenstein, MD.
N.K. often happens after an infection or trauma to the head or neck. Brain and skull base tumors are also common causes of N.K. Failing to blink can damage the cornea, causing cloudy and blurry vision. Typical treatment includes eye drops and surgery to permanently close a portion of the eye to protect it.
Dr. Rubenstein further explains, “All of those are supportive and none of them really get at the underlying problem, which is the nerve damage itself.”
Now a team of surgeons at UNC hospitals are performing corneal neurotization. During the surgery, healthy nerve is taken from the lower leg and used to re-connect the healthy nerve just beneath the eyebrow to the damaged cornea.
“Those nerves actually grow back into the damaged cornea and replace the nerves that are no longer functioning,” mentions Dr. Rubenstein.
It takes patients up to six months to notice improved vision and sensation. The healing process is slow, but can be life changing.
Contributors to this news report include: Marsha Lewis, Producer; Matt Goldschmidt, Videographer & Editor.
To receive a free weekly e-mail on medical breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
Source:
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TITLE: EYES WIDE OPEN: BREAKTHROUGH BLINK RESTORATION
REPORT: MB #5358
BACKGROUND: Neurotrophic keratitis (NK), also known as neurotrophic keratopathy, is a rare degenerative disease of the cornea caused by damage to the trigeminal nerve, which supplies sensory innervation to the cornea. This condition leads to impaired corneal sensitivity and reduced tear production, resulting in poor corneal healing and potential vision loss if left untreated. Because NK is rare, it only affects about 5/10,000 of people. Neurotrophic keratitis can be caused by herpes simplex virus infection, herpes zoster, diabetes, long-term use of certain medications such as topical ocular medications or contact lenses.
(Sources: https://rarediseases.org/rare-diseases/neurotrophic-keratitis/
https://www.ncbi.nlm.nih.gov/books/NBK431106/
https://dryeyespecialist.com/neurotrophic-keratitis/)
DIAGNOSING: The symptoms of neurotrophic keratitis can vary depending on the severity of the condition but may include redness, foreign body sensation – like feeling like an eye lash or a grain of salt is in your eye – blurred vision, sensitivity to light, and/or mucus discharge from the eye. Diagnosis of neurotrophic keratitis typically involves a comprehensive eye examination, including measurement of corneal sensitivity using specialized instruments such as a Cochet-Bonnet aesthesiometer. Other diagnostic tests may include corneal staining with vital dyes, such as fluorescein, to assess the integrity of the corneal surface.
(Sources: https://dryeyespecialist.com/neurotrophic-keratitis/
https://eyewiki.aao.org/Neurotrophic_Keratitis#Symptoms)
NEW TECHNOLOGY: A new procedure out of the University of North Carolina at Chapel Hill is proving to help patients with this condition. According to the press release, “The goal of the corneal neurotization surgery is to transfer a nearby healthy nerve to the damaged cornea to restore its sensation. After approximately six months, the patient may start to notice improved sensation and, ultimately, vision. The healing process is slow but life changing for patients.
The surgery’s minimally invasive nature is especially important for patients because it reduces scarring on the face, numbness and other potential side effects.”
(Source: https://www.unc.edu/discover/new-procedure-restores-vision/)
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
Kendall Daniels
Kendall.daniels@unchealth.unc.edu
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com