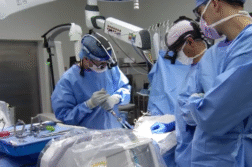
CHICAGO, Ill. (Ivanhoe Newswire)— Spinal surgery is a last resort when medications and non-surgical treatments are not working. The surgery itself must be precise to get the best outcomes. Now there’s a new FDA-approved augmented reality device that’s helping surgeons have a more accurate and faster surgery—translating to a better recovery for patients. Details on the device that is bringing AR to the OR.
Being able to do this is a big triumph for Paul Zakula. Fourteen years ago, back pain slowed him down. He had a fusion, but the pain came back years later.
“When it got bad, it got bad. It got to the point, really, where I could not even walk ten steps anymore,” shared Zakula.
Paul went to his doctor and got an MRI.
“Sat down and he stuck it in the computer, and he was just staring at it, not saying a word, which I knew that couldn’t be good,” recalled Zakula.
He was going to need spine surgery again. But this time, his surgeon had a new tool for a better surgery. This headset called x-vision is a surgical guidance system that allows the surgeon to see through Paul’s skin as if he had x-ray vision.
“What it enables us to do is place screws through tiny poke incisions with 3D visualization of the spine,” explained Frank Phillips, MD, a professor of orthopedics at Midwest Orthopedics at Rush.
CT scans are displayed right in front of the surgeon’s eyes in real time, keeping the surgeon’s focus on the patient instead of looking away to see scans on a separate monitor. The device allows the surgery to be more accurate and efficient.
“Place screws in five vertebrae in under half an hour using pre-augmented reality techniques that would often take double that amount of time,” illustrated Dr. Phillips.
Quicker and safer surgery means faster recovery. For Paul, six weeks after his surgery …
“I’m able to get up every morning and walk for an hour,” expressed Zakula.
Leaving his back pain behind him.
Right now, the device is approved to only be used in spinal surgery, but Augmedics, the company that designed the headset, has future plans to use this for other surgeries.
Contributors to this news report include: Cyndy McGrath, Executive Producer; Milvionne Chery, Field Producer; Kirk Manson, Videographer; Roque Correa, Editor.
To receive a free weekly e-mail on Medical Breakthroughs from Ivanhoe, sign up at: http://www.ivanhoe.com/ftk
MEDICAL BREAKTHROUGHS
RESEARCH SUMMARY
TOPIC: augmented reality for spine surgery
REPORT: MB #4800
THE SPINE: The spine is a column of 26 bones in an adult body. Twenty-four separate vertebrae interspaced with cartilage, and then additionally the sacrum and coccyx. There are five major regions of the spine. The cervical which is the seven vertebrae in the neck, the thoracic which is the 12 vertebrae in the chest region, the lumbar which are the five vertebrae in the lower back, the sacral which contains only the sacrum and is a single bone in the adult skeleton that is formed by the fusion of five smaller vertebrae during adolescence. It is a flat, triangular bone found in the lower back and wedged between the 2 hip bones. Finally, the coccygeal which is known as the human tailbone and contains only the coccyx which is formed by the fusion of four tiny vertebrae during adolescence.
(Source: https://www.innerbody.com/image/skel05.html#continued)
TRADITIONAL SPINAL FUSION SURGERY: A spinal fusion surgery is designed to stop the motion at a painful vertebral segment, which in turn should decrease pain generated from the joint. There are many approaches to lumbar spinal fusion surgery, and all involve adding bone graft to a segment of the spine, setting up a biological response that causes the bone graft to grow between the two vertebral elements to create a bone fusion and the boney fusion – which results in one fixed bone replacing a mobile joint – stops the motion at the joint segment. The procedure for Spine Fusion using the TLIF (Transforaminal Lumbar Interbody Fusion) back surgery is done through the posterior (back) part of the spine. Surgical hardware is applied to the spine to help enhance the fusion rate. Pedicle screws and rods are attached to the back of the vertebra and an interbody fusion spacer is inserted into the disc space from one side of the spine. Then a bone graft is obtained from the patient’s pelvis and is placed into the interbody space and alongside the back of the vertebra to be fused. As the bone graft heals, it fuses the vertebra above and below and forms one long bone.
(Source: https://www.spine-health.com/treatment/spinal-fusion/lumbar-spinal-fusion-surgery)
NEW TECHNOLOGY: The Augmedics Xvision, Spine System surgical guidance system allows a surgeon to see a patient’s 3-dimensional (3D) spinal anatomy through skin as if they have x-ray vision. The Xvision system is revolutionizing how surgery is performed by giving the surgeon better control and visualization, which can lead to easier, faster, and safer surgeries. “Having 3-dimensional (3D) spinal anatomic and 2-dimensional (2D) CT scan images directly projected onto the surgeon’s retina and superimposed over the surgical field takes spinal surgery to another level,” said Dr. Frank Phillips, Professor and Director of the Division of Spine Surgery and the Section of Minimally Invasive Spine Surgery at Rush University Medical Center. “Being able to place minimally invasive spinal instrumentation extremely accurately and efficiently, reducing surgical time and complication risk, is critical to improving outcomes for spinal surgery. Traditional surgical navigation platforms have been shown to improve accuracy of implant placement, however using augmented reality allows for the advantages of traditional (non-3D) navigation plus the ability to visualize the patients spinal anatomy in 3D through the skin.”
FOR MORE INFORMATION ON THIS REPORT, PLEASE CONTACT:
ANN PITCHER
If this story or any other Ivanhoe story has impacted your life or prompted you or someone you know to seek or change treatments, please let us know by contacting Marjorie Bekaert Thomas at mthomas@ivanhoe.com