DALLAS, Texas (Ivanhoe Newswire) — It’s called Achalasia, where people lose the ability to swallow. It’s far more serious than heartburn, acid reflux, and GERD, and can lead to death. But a new, less invasive technique is making it possible for patients to swallow again.
On her way back to college, 51-year-old Jennifer Smilie has had trouble swallowing food.
“When I would eat regular food, I would immediately have like a choking feeling and would have to run to the nearest bathroom to vomit the food that was stuck,” Jennifer explained.
Turns out what she thought was acid reflux, was actually a rare condition called Achalasia, where the bottom muscle of her esophagus would not open to allow food to enter her stomach. Most people lose weight, but Jennifer consumed nothing but milkshakes that caused her to become obese. Now a new technique will allow her to eat solid foods again.
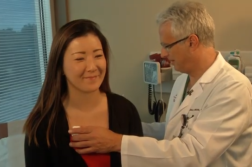
“I think it’s one of the biggest advances we’ve had in esophageal surgery in a long time,” shared Steven Leeds, MD, FACS, Division Chief of Minimally Invasive Surgery at Baylor Scott & White Health.
Dr. Leeds applied an advanced technique called “POEM”, peroral endoscopic myotomy, to open up the bottom of her esophagus through her mouth, instead of cutting into her abdomen.
“No incisions on her, no recovery time, and no pain,” said Dr. Leeds.
Before the POEM procedure, Jennifer underwent gastric bypass surgery and lost 130 pounds. Now, she can eat whatever she wants.
“It’s been life-changing for me. I no longer have any reflux, I don’t have to worry about where the nearest bathroom is, I can eat in wonderful moderation anything that I want to eat,” stated Jennifer.
Including spicy foods.
“Yes, I do. I do like spicy food,” smiled Jennifer.
The “POEM” technique is not available in every hospital, so people who suffer with Achalasia should consult a specialist and ask specifically about the peroral endoscopic myotomy.
Contributors to this news report include: Don Wall, Producer; Roque Correa, Editor; and Matt Goldschmidt, Videographer.
TROUBLE SWALLOWING: ACHALASIA
REPORT #2777
BACKGROUND: Achalasia is a rare disorder of the esophagus, which is the tube that carries food from the throat to the stomach. It is the impaired ability to push food down toward the stomach, failure of the ring-shaped muscle at the bottom of the esophagus, the lower esophageal sphincter (LES), to relax. What typically moves food through the esophagus is the contraction and relaxation of the sphincter. The exact cause of achalasia is not known. Some clinical researchers suspect that the condition may be caused by the degeneration of a group of nerves located in the chest. It is believed that there may be a rare, inherited form of achalasia, but this is not yet well understood.
(Source: https://rarediseases.org/rare-diseases/achalasia/#:~:text=Achalasia%20is%20a%20rare%20disorder,(LES)%2C%20to%20relax and
DIAGNOSIS OF ACHALASIA: Patients usually describe a worsening in swallowing (dysphagia) of solid and liquid food over a period of many months. They may experience regurgitation of food, chest pain, or loss of weight. Because patients typically learn to compensate for their swallowing by taking smaller bites, chewing well, and eating slowly, the diagnosis of achalasia often is delayed by months or even years. This delay is unfortunate because early treatment could prevent esophageal dilation and its complications. The dysphagia in achalasia is different from the dysphagia of esophageal stricture (narrowing of the esophagus due to scarring) and esophageal cancer. In achalasia, dysphagia usually occurs with both solid and liquid food, whereas in esophageal stricture and cancer, the dysphagia typically occurs only with solid food and not liquids, until very late in the progression of the stricture.
(Source: https://www.medicinenet.com/achalasia/article.htm#how_is_achalasia_diagnosed)
TREATMENT APPROACH: Treatments for achalasia focuses on relaxing, or stretching open, the lower esophageal sphincter. This allows food and liquid to move more easily through the digestive tract. Some nonsurgical options include pneumatic dilation. It is where a balloon is inserted by endoscopy into the center of the esophageal sphincter and inflated to enlarge the opening. This outpatient procedure may need to be repeated. Another option is Botox. This muscle relaxant is injected directly into the esophageal sphincter with an endoscopic needle. It’s generally recommended for people who aren’t good candidates for pneumatic dilation or surgery. Or, your doctor might suggest muscle relaxants such as nitroglycerin (Nitrostat) or nifedipine (Procardia) before eating. Some surgical options are a heller myotomy. This is where the surgeon cuts the muscle at the lower end of the esophageal sphincter to allow food to pass more easily into the stomach. To avoid future problems with GERD, a procedure known as fundoplication might be performed at the same time. Another option is a peroral endoscopic myotomy (POEM). In this procedure, the surgeon uses an endoscope inserted through the mouth and down the throat to create an incision in the inside lining of the esophagus. Then, the surgeon cuts the muscle at the lower end of the esophageal sphincter.
(Source: https://www.mayoclinic.org/diseases-conditions/achalasia/diagnosis-treatment/drc-20352851)
* For More Information, Contact:
Steven Leeds, MD Matthew Olivolo
CASClinicalOps@bswhealth.org matthew.olivolo@bswhealth.org
Free weekly e-mail on Medical Breakthroughs from Ivanhoe. To sign up: http://www.ivanhoe.com/ftk