SAN FRANCISCO, Calif. (Ivanhoe Newswire) — In the last four decades, the survival rate for children diagnosed with cancer has jumped from ten percent to a whopping 90 percent. While those numbers are remarkable, many patients still face eventual problems from the effects of chemotherapy. As a result, a hospital in San Francisco has made sure these kids will have a team in their corner, long after the cancer is gone.
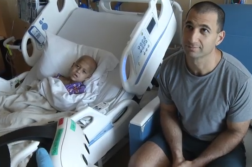
Gertie is as energetic and carefree as any five-year-old can be. And mom, Jeni Jensen, couldn’t be happier.
On Gertie’s first birthday she was diagnosed with acute myeloid leukemia, a rare form of cancer. The chances of being diagnosed with it are greater for kids with Down syndrome, like her.
“It’s such a scary diagnosis. I mean you’re faced with mortality with your child,” Jenson shared.
Gertie beat it, but the risk isn’t completely gone. Sixty percent of survivors face long-range side effects from chemo, including infertility, heart issues and other cancers.
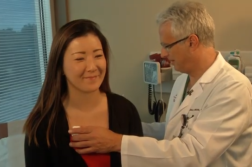
“So, we need to make sure we’re monitoring their care long-term,” Robert Goldsby, MD, UCSF Benioff Children’s Hospital in San Francisco told Ivanhoe.
And that’s exactly what the survivor’s clinic at UCSF is doing. A team of nurses, nutritionists, social workers and oncologists work together to track a child’s health long into adulthood.
Dr. Goldsby continued, “I’ve seen patients older than me. We see them life-long, as long as they’re willing to come.”
Social workers evaluate patients’ mental well-being. Nutritionists focus on eating habits. And physical exams help predict long-term health.
“And then we have a referral group, that if they need a geneticist or they need a cardiologist,” explained Dr. Goldsby.
All of the patient’s health information is then summed in a wallet size “survivor’s health passport” for any doctor to review.
Jensen said, “The passport is awesome. It has all the information that they need to look for possible side effects from her chemotherapy.”
But the best part of it all, Gertie is showing no signs of complications.
“All the support is so important. She’s a blessing,” Jensen said beaming.
Patients in the survivor’s clinic still need to see a primary care physician for routine check-ups. And it’s recommended that they join the program two years after becoming cancer free. That’s when the risk of a reoccurrence is reduced and doctors can begin looking for side effects.
Contributors to this news report include: Jennifer Winter, producer; Roque Correa, Editor and Rusty Reed, Videographer.
Free weekly e-mail on Medical Breakthroughs from Ivanhoe. To sign up: http://www.ivanhoe.com/ftk
CLINIC FOR CHILDHOOD CANCER SURVIVORS
REPORT #2513
BACKGROUND: Childhood cancer (also called pediatric cancer) typically means a cancer that is found in children and teens, and sometimes young adults. There are many types, which can be found in different places throughout the body. The most common cancer in children is leukemia, a type of blood cancer. Cancer can also occur in organs and tissues such as the lymph nodes, nervous system and muscles, bone and skin. Cancer is diagnosed each year in about 175,000 children ages 14 and under worldwide. It is the leading cause of death by disease past infancy for U.S. children. However, thanks to better therapies, more than 80 percent of U.S. childhood cancer patients now become long-term survivors. Survival rates can vary depending on the type of cancer. About 420,000 childhood cancer survivors live in the U.S., with many more around the world.
(Source: https://www.stjude.org/treatment/pediatric-oncology/childhood-cancer-facts.html)
CAUSES OF CANCER IN CHILDREN: The causes of childhood cancer are not completely understood. While adult cancers are often linked to lifestyle or environmental factors, cancer in children is different in several ways. In a young person, cancer is less likely to be caused by the patient’s environment or lifestyle. Instead, cancer-causing genetic changes, or mutations, are most commonly thought to occur by chance. However, in a few cases children are born with genetic changes that increase their risk of getting cancer. Learning what genetic changes caused a cancer can help doctors diagnose it more effectively. Going forward, this information may also help scientists develop better treatments. Robert Goldsby, MD, Pediatric Oncologist with UCSF Benioff Children’s Hospital in San Francisco, shared, “Kids with Down Syndrome are at higher risk of both acute myelogenous leukemia (AML) and acute lymphoblastic leukemia (ALL). ALL is the most common form of cancer in children in general.”
(Source: https://www.stjude.org/treatment/pediatric-oncology/childhood-cancer-facts.html)
CANCER RESEARCH MAKING BREAKTHROUGH: The Food and Drug Administration approved a groundbreaking cancer treatment for childhood leukemia that uses patients’ genetically altered immune cells to fight the disease. It is the first gene therapy to be cleared in the United States, and one with major ramifications for patients with cancer as well as other diseases. The decision gave the green light to the Novartis drug, Kymriah, for children and young adults whose leukemia doesn’t respond to traditional approaches. The one-time, customized treatment is also being tested for a range of diseases from non-Hodgkin lymphoma and multiple myeloma to solid tumors. “We’re entering a new frontier in medical innovation with the ability to reprogram a patient’s own cells to attack a deadly cancer,” FDA Commissioner Scott Gottlieb said. Unlike some experimental gene approaches, the Novartis treatment, called CAR T-cell therapy, doesn’t replace disease-causing genes with healthy ones. Instead, in a complicated and personalized process, white blood cells called T cells are extracted from the patient and sent to a manufacturing center to be altered to include a new gene that directs the T cells to target and kill leukemia cells. Those T cells, an important part of the immune system, are then infused back into the patient. Carl June, the University of Pennsylvania professor who led the treatment’s development, said he believes it will be a game-changer not just for children with leukemia, but potentially for all cancer patients.
ADDITIONAL LINK: https://www.alexslemonade.org/blog/2017/06/five-childhood-cancer-researchers-making-breakthroughs
* For More Information, Contact:
Robert Goldsby, MD – USF Suzanne Leigh, University Relations
GoldsbyR@ucsf.edu suzanne.Leigh@ucsf.edu, (415) 476-2993