RALEIGH, N.C. (Ivanhoe Newswire) — Can stimulating electrical activity in the brain help the millions of people who suffer from disorders like depression and chronic pain? Researchers who are studying the effects on humans say the results are very promising!
Electrical engineer Flavio Frohlich went from working with computers to something more complex.
“There’s a much more fascinating device out there and that’s the brain,” shared Flavio Frohlich, PhD, Director, Carolina Center for Neurostimulation, UNC School of Medicine.
The professor says, similar to computers, our body generates electrical signals.
“The goal is to understand the electric signaling, to understand what the brain is trying to tell us,” continued Frohlich.
Graduate student and doctoral candidate at UNC School of Medicine, Julianna Prim is studying chronic pain in military personnel. She and Frohlich met and sparked an idea!
“Stimulate the brain with TACS, which is transcranial alternating current stimulation,” Prim explained.
Researchers conducted studies using a weak alternating electrical current.
“We’re attaching electrodes to the scalp. We pass minute, tiny amounts of electricity through these electrodes,” said Frohlich.
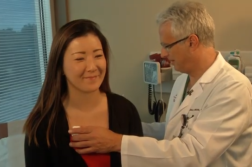
Julianna demonstrates with a mock patient how the process works.
The patient is asked to relax while looking at a soothing image.
“There’s a very slight tingling at the back of my head, but it’s very subtle,” explained Chris Walker, postdoctoral researcher at UNC School of Medicine.
In a pilot study of 20 participants, the results were very encouraging.
Prim told Ivanhoe, “We found that there was an increase in pain improvement compared to the placebo stimulation.”
Both believe this could lead to non-invasive treatments for different brain disorders.
“By adjusting the stimulation to match specific changes in those brains,” concluded Frohlich.
Giving millions of people suffering, hope.
The UNC researchers have submitted a grant to expand the chronic pain study to 120 patients to find out how long the effects last. The hope is the stimulation device would one day be available for patients to use at home. They also conducted a TACS study for depression and found 70 percent of participants reported improvement in symptoms. Studies on electrical brain stimulation for schizophrenia and lupus patients are about to get underway. For more information, go to www.carolinaneurostimulation.org or www.frohlichlab.org.
Contributors to this news report include: Janna Ross, Field Producer; Roque Correa, Editor; and Kirk Manson, Videographer.
BRAIN STIMULATION: TREATING DEPRESSION AND CHRONIC PAIN
REPORT #2732
BACKGROUND: Over the course of a year, major depressive disorder affects approximately 17.3 million American adults, or about 7.1% of the U.S. population age 18 and older. Major depressive disorder is more prevalent in women than in men. Approximately 1.9 million children ages 3 to 17 have been diagnosed with depression. One of the most common reasons adults seek medical care is chronic pain, which has been linked to restrictions in mobility and daily activities, dependence on opioids, anxiety and depression, and poor perceived health or reduced quality of life. Population-based estimates of chronic pain among U.S. adults range from 11% to 40%. When you experience chronic pain along with depression, it’s even tougher. Depression magnifies pain and makes everyday living more difficult. It’s important to know that medications and psychotherapy can help relieve the depression and make chronic pain more tolerable.
(Source: https://www.dbsalliance.org/education/depression/statistics/ and https://www.cdc.gov/mmwr/volumes/67/wr/pdfs/mm6736a2-H.pdf and https://www.webmd.com/depression/guide/depression-chronic-pain#1)
TREATING BOTH PAIN AND DEPRESSION: Pain specialists will treat both chronic pain and depression together, often with the same techniques, which include progressive muscle relaxation, hypnosis, and meditation. Physicians will usually prescribe standard medications like acetaminophen, aspirin and other nonsteroidal anti-inflammatory drugs. In severe cases, they will prescribe opiates along with a variety of psychiatric drugs. Physical therapists provide exercises not only to break the vicious cycle of pain and immobility, but also to help relieve depression. Cognitive and behavioral therapies teach pain patients how to avoid fearful anticipation, clear discouraging thoughts, and adjust everyday routines to ward off physical and emotional suffering. Psychotherapy helps demoralized patients and their families tell their stories and describe the experience of pain in its relation to other problems in their lives. Pain specialists can improve their practice by learning more about the interactions among psychological, neurological, and hormonal influences that link pain and depression.
(Source: https://www.health.harvard.edu/mind-and-mood/depression-and-pain)
NEW STUDY COMBINES TREATMENT: A randomized controlled study, the Stepped Care for Affective Disorders and Musculoskeletal Pain (SCAMP), suggests that a combination approach might work for people suffering pain in addition to a psychiatric disorder. The study enrolled 250 patients with chronic pain in the lower back, hip, or knee, along with moderate depression, as measured by a standard clinical instrument. One group was assigned to 12 weeks of antidepressant therapy followed by a 12-week pain self-management intervention based on principles of cognitive behavioral therapy. Results were considered significant if participants reported at least a 50% reduction in depression severity and at least a 30% reduction in pain. At the 12-month mark, both depression and pain were significantly reduced in 32 of 123 intervention patients, compared with 10 of 127 participants in the “usual care” or control group.
(Source: https://www.health.harvard.edu/mind-and-mood/pain-anxiety-and-depression)
* For More Information, Contact:
Flavio Frohlich, PhD Mark Derewicz, PR UNC Chapel Hill
Flavio_frohlich@med.unc.edu mark.derewicz@unchealth.unc.edu
Free weekly e-mail on Medical Breakthroughs from Ivanhoe. To sign up: http://www.ivanhoe.com/ftk