Seattle, Wash. (Ivanhoe Newswire) — Most people who have it say they wouldn’t wish it on their worst enemies. It’s chronic pain and best estimates say a hundred million Americans suffer from it every day all day. Many turn to surgery and pain meds, but a Seattle doctor says we’ve got it all wrong.
It’s music for Charley Pavlosky: the sound of a solid tee shot on the back nine. Even sweeter today than just a few years ago: competing in the U.S. Open. Chronic pain stole away his favorite sport.
“Imagine the worse tooth ache you’ve ever had and it being your whole body 24 hours a day, and you cannot stop it,” Pavlosky told Ivanhoe.
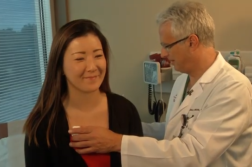
After seeing countless doctors, Pavlosky found an ally in Seattle-based spine surgeon, David Hanscom, MD. He believed the root of Pavlosky’s pain was not an old back injury, but a fired up nervous system. Surgery was not the answer.
Dr. Hanscom detailed, “I see patients every week that have major complications from surgeries that probably never should have been done. Chronic pain is a neurological problem.”
How so? Our brains are designed to memorize pain that lasts for three months or longer. Once that happens, the ache may feel the same but it is now controlled by our nervous system, not the original injury.
Dr. Hanscom continued, “About five years ago my staff took that seriously. So it started with every patient that we would address sleep, stress, balance medications.”
Along with recommending better diet and exercise, Dr. Hanscom said the pain fades. For Pavlosky, that was better than a hole in one.
“I have zero pain and that’s most of the time,” said Pavlosky.
In the last two years, 97 Dr. Hanscom patients have canceled their surgeries after their pain vanished. Now to help more people, Dr. Hanscom has a book out, called Back in Control’.
“Within three to six months, 90 percent of people get better without surgery,” Dr. Hanscom told Ivanhoe.
Pavlosky said, “I came to see a doctor and I wound up meeting a healer. And that was an extraordinary awakening moment.”
Dr. Hanscom said one of the most effective ways to keep our nervous system calm and avoid pain is through expressive writing. Simply write down what’s on your mind and then tear it up. Doing this helps separate you from your thoughts and creates a sense of peace. The doctor credits this exercise with helping him get out of his own pain years ago.
Contributors to this news report include: Jennifer Winter, Producer; Evan Borders, Photographer; Robert Walko, Editor.
Free weekly e-mail on Medical Breakthroughs from Ivanhoe. To sign up: http://www.ivanhoe.com/ftk
BACK IN CONTROL: ALTERNATIVES TO BACK SURGERY
REPORT #2496
BACKGROUND: While acute pain is a normal sensation triggered in the nervous system to alert you to possible injury and the need to take care of yourself, chronic pain is different. Chronic pain persists. Pain signals keep firing in the nervous system for weeks, months, even years. Chronic pain affects more Americans than diabetes, heart disease and cancer combined. It is a leading cause of disability and is a major contributor to health care costs. According to the National Center for Health Statistics, approximately 76.2 million Americans have suffered from pain that lasts longer than 24 hours and millions more suffer from acute pain. Chronic pain is the most common cause of long-term disability. Pain can be a chronic disease, a barrier to cancer treatment, or can occur alongside other diseases and conditions like depression, post-traumatic stress disorder, and even traumatic brain injury. For infants and children, pain requires special attention, particularly because they are not always able to describe the type, degree, or location of pain they are experiencing.
(Source: http://www.painmed.org/patientcenter/facts_on_pain.aspx and https://report.nih.gov/nihfactsheets/ViewFactSheet.aspx?csid=57)
SYMPTOMS AND CURRENT TREATMENTS: Chronic pain may arise from an initial injury, such as a back sprain, or there may be an ongoing cause, such as illness. However, there may also be no clear cause. Other health problems, such as fatigue, sleep disturbance, decreased appetite, and mood changes, often accompany chronic pain. Chronic pain may limit a person’s movements, which can reduce flexibility, strength, and stamina. The goal of treatment is to reduce pain and improve function, so the person can resume day-to-day activities. Patients and their healthcare providers have a number of options for the treatment of pain. Whatever the treatment plan, it is important to remember that chronic pain usually cannot be cured, but it can be managed. Some of the most common ways to manage pain are with medications, acupuncture, electrical stimulation, nerve blocks, or surgery. Self-management holds great promise as a treatment approach. In self-management programs, the individual patient becomes an active participant in his or her pain treatment engaging in problem-solving, pacing, decision-making, and taking actions to manage their own pain. Finally, behavioral interventions for pain demonstrate promise for providing pain relief either in conjunction with or in lieu of drug interventions.
(Source: https://medlineplus.gov/magazine/issues/spring11/articles/spring11pg5-6.html and https://report.nih.gov/nihfactsheets/ViewFactSheet.aspx?csid=57)
BREAKTHROUGH IN ADOLESCENT CHRONIC PAIN: A University of Calgary psychologist who studies pediatric pain has made a breakthrough in understanding the cause of chronic pain in adolescents by focusing on those recovering from major surgeries. Melanie Noel, an assistant professor in the Department of Psychology and a member of the Alberta Children’s Hospital Research Institute, has found that adolescents’ memories of pain following major surgeries influences their recovery and may lead to the development of chronic pain, or pain that persists beyond the expected time of healing. Noel and her co-authors state that psychological and language-based interventions may be used to help adolescents better cope with their post-surgical pain, thus reframing their memories of the pain and potentially altering the path that can lead to chronic pain. The study could have huge implications given that 15 to 40 percent of youth experience chronic pain. Studies have also shown that 60 percent of children with chronic pain will become adults with chronic pain and mental health disorders.
* For More Information, Contact:
David Hanscom, MD Beth Grossman
Swedish Neuroscience Institute bethgrossman555@gmail.com
dnhanscom@gmail.com 212-949-4071