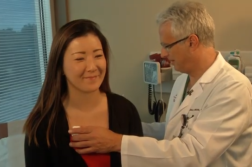
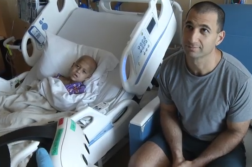
ORLANDO, Fla. (Ivanhoe Newswire) — There are about 50 million surgical procedures performed every year in the United States. However, many people do not follow doctor’s orders after surgery. Here are tips on how you can keep your recovery on track and avoid costly mistakes.
Going under the knife already has its risks, but not following the proper recovery procedure can be even riskier. Mistake number one is staying in bed too long.
“Making sure that we get them up and walking around to avoid things like blood clots and pneumonias is critically important,” says Scott Steele, MD, MBA, Department of Colorectal Surgery, Cleveland Clinic.
As soon as the doctor has cleared you to move around, do it. A little physical activity also wakes up your gut.
“Their bellies are able to wake up faster, they feel better faster and they’re able to get home sooner,” continued Dr. Steele.
But also make sure you’re not doing too much too soon. If the doctor clears you to walk a little every day that may not necessarily mean that you can start lifting 30 pound boxes. Pay attention to the doctor’s do’s and don’ts. If you overdo it, it may set you back in your recovery. One final mistake to avoid, is not taking your meds as prescribed. According to the CDC, about 30 percent of prescriptions are never filled and 50 percent are not taken as prescribed. Staying on top of your meds during recovery will keep you out of the hospital and your recovery on track.
Another thing to be careful of is getting behind the wheel after surgery. Your reaction time may be slower and that can get you into an accident. So don’t drive until your doctor has cleared you.
Contributors to this news report include: Milvionne Chery, Field Producer; Roque Correa, Editor.
Free weekly e-mail on Medical Breakthroughs from Ivanhoe. To sign up: http://www.ivanhoe.com/ftk
AVOID THESE RECOVERY MISTAKES
REPORT #2646
BACKGROUND: There are approximately 234 million major surgeries performed each year around the world. That means one out of 25 people will have a major surgery in a given year. More than 25 percent of these surgeries are performed to treat injuries sustained in a traumatic accident. Recovering from surgery is greatly dependent upon the type of surgery you will be having. An outpatient procedure, such as a hand surgery, will have a far different recovery period than an invasive, inpatient procedure, such as a heart bypass surgery. The level of activity permitted varies widely with the procedure performed. Some surgeries, such as a hip replacement, may require physical therapy while other patients may be discharged with instructions to “take it easy.” Pain after surgery is a good indication of whether or not the patient is trying to do too much. It should be manageable with the prescribed pain medication. Experiencing no pain is often an unreasonable expectation, but pain should be controlled enough to allow walking to the bathroom, sitting up in a chair and coughing.
(Source: https://www.wisegeek.com/how-many-surgeries-are-performed-each-year.htm and https://www.verywellhealth.com/recovering-from-surgery-what-to-expect-3156826)
RECOVERING FROM SURGERY: Patients who are physically able will be expected to walk or sit on the edge of the bed as soon as they are able. This activity is essential to prevent complications including deep vein thrombosis. Deep coughing, commonly referred to as “a cough and deep breathe,” is encouraged at this time. Coughing expands the lungs and helps prevent pneumonia and other breathing difficulties patients face after surgery. Incision care is very important after surgery, as well. Depending on the nature of the surgery, the bandage may be changed frequently or only when ordered by the surgeon. A common result of pain medication and anesthesia is constipation and difficulty urinating, so clear fluids will be encouraged and a mild stool softener may be prescribed by the surgeon. If the patient is unable to empty his/her bladder, a catheter may be reinserted. Once the digestive system is moving again the patient is typically allowed to begin a clear liquid diet and progress to a normal diet.
(Source: https://www.verywellhealth.com/recovering-from-surgery-what-to-expect-3156826)
PARTNERING WITH PATIENTS: At NYU School of Medicine, Adina Kalet, MD, MPH, professor of medicine and surgery and co-director of the Program on Medical Education Innovation and Research, is exploring the use of a Patient Empowerment Program to help patients become more active partners in their care. In a current study, she and colleagues are training patients with diabetes to better communicate with physicians. For Steven Feldman, MD, PhD, professor of dermatology, pathology, and public health sciences at Wake Forest Baptist Medical Center, close follow-up and establishing trust with patients are the keys to patient adherence. Prescribing a drug and then following up in 8 to 12 weeks is not enough to ensure compliance, he said. “Doctors are the only people on the planet who have the idea that you can tell people, ‘Here, work on this every day and I’ll see you in two or three months.’” Feldman has found that being a caring provider leads to better patient accountability.
(Source: https://news.aamc.org/patient-care/article/patients-follow-doctors-advice-better-outcomes/)
* For More Information, Contact:
Caroline Auger