TAMPA, Fla. (Ivanhoe Newswire) — You probably know about brain aneurysms, but how about abdominal aneurysms? They mainly target white men 65 years old and older, but women can also get them. Next, learn about the risk factors you need to look out for and the new device some doctors say could add years to your life.
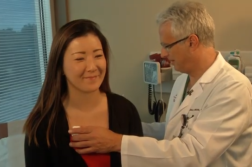
After 52 years of marriage, Michael and Elaine Renner still find the joy in life.
But a series of tests last year brought bad news. Michael had an abdominal aortic aneurysm also known as triple-A. Doctors were direct: if it ruptures, you’ll probably die.
“Talking to the doctors they said this is life or death here you’ve got to have it fixed,” Michael shared.
These aneurysms happen when a spot on the body’s largest artery, the aorta, weakens and expands. Michael’s doctors told him his only hope was an experimental device only a few doctors are testing.
Murray Shames, MD, Vascular Surgeon at USF Health told Ivanhoe, “This is a physician sponsored trial approved by the FDA, approved by Medicare and would be reimbursed by your insurance carrier.”
Guided by x-rays, doctors assemble what’s known as the Patrick Kelly device over the bulging aorta to prevent it from rupturing. There are risks and USF is only one of only six sites in the country testing it.
“We do like to take precaution with the spinal cord there is still some risk that you could get a spinal cord injury and end up with paralysis. The risk is significantly lower than getting open traditional surgery,” Dr. Shames continued.
“He did a great job,” Michael said.
Now Michael is back enjoying life with Elaine.
“We are very grateful that we have this. And basically it’s a new lease on life,” Elaine added.
At 73 years old, doctors say he has lots of life to live.
Abdominal aortic aneurysms are called silent killers because they usually cause no symptoms. They are often found during a routine exam. Triple A’s run in families and doctors say screening could save the life of someone you love.
Contributors to this news report include: Sarah Rosario, Field Producer; Roque Correa, Editor; and Angela Claney, Videographer.
Free weekly e-mail on Medical Breakthroughs from Ivanhoe. To sign up: http://www.ivanhoe.com/ftk
ABDOMINAL ANEURYSMS: SILENT KILLERS
REPORT #2607
BACKGROUND: An abdominal aortic aneurysm (AAA) is an enlarged area in the lower part of the aorta, the major blood vessel that supplies blood to the body. AAA is the 13th leading cause of death in the U.S. “All men age 65 and older should get an abdominal ultrasound screening as a welcome to Medicare patient,” says Marcelo Giarelli, MSN, RN, CCRN, Tampa General Hospital. “Ruptures are life-threatening and 50% die spontaneously and 50% of the patients who do survive to get to a hospital will expire. There is a 75%-80% mortality rate,” Giarelli continued. Once an AAA is found, doctors will closely monitor it so that surgery can be planned if it’s necessary. Emergency surgery for a ruptured AAA can be risky. Aortic aneurysms were the primary cause of 9,863 deaths in 2014 and a contributing cause in more than 17,215 deaths in the United States in 2009. About two-thirds of people who have an aortic dissection are male.
SIGNS AND SYMPTOMS: AAA’s are usually asymptomatic until they expand or rupture. Patients may experience unimpressive back, flank, abdominal, or groin pain for some time before rupture. At times, AAA’s may cause symptoms from local compression, including nausea, vomiting, urinary symptoms, or venous thrombosis from venous compression. Back pain can be caused by erosion of the AAA’s into adjacent vertebrae. Other symptoms include embolic phenomena affecting the toes. Patients may describe a pulse in the abdomen and may actually feel a pulsatile mass. It is important to note progressive symptoms, which should alert the clinician to the possibility of expansion with imminent rupture. An expanding AAA commonly causes sudden, severe, and constant low back, flank, abdominal, or groin pain. Syncope may be the chief complaint, with pain less prominent. Patients with a ruptured AAA may present in frank shock, as evidenced by cyanosis, mottling, altered mental status, tachycardia, and hypotension. As many as 65% of patients with ruptured AAA’s die of sudden cardiovascular collapse before arriving at a hospital. Dr. Patrick Kelly designed and invented the device (Sanford Health) which has been available to us for 1 year but was actually developed before that. The device is manufactured by Medtronic Healthcare Company and is officially called the Valiant Thoracoabdominal Stent Graft.
(Source: https://emedicine.medscape.com/article/1979501-clinical#b1 and Marcelo Giarelli, MSN, RN, CCRN, Tampa General Hospital)
THE FORECAST OF “AAA’S”: A new approach that distills deluges of genetic data and patient health records has identified a set of telltale patterns that can predict a person’s risk for this common, and often fatal, cardiovascular disease, according to a new study from the Stanford University School of Medicine. Although the method, which uses a form of artificial intelligence called machine learning, has so far only been used to predict the likelihood of this particular condition, called abdominal aortic aneurysm, it’s proof that such an approach could decipher the molecular nuances that put people at risk for just about any complex genetic disease. “Right now, genome sequencing is starting to make its mark,” said Michael Snyder, PhD, professor and chair of genetics at Stanford. “It’s being used a lot in cancer, or to solve mystery diseases. But there’s still a big open question: How much can we use it for predicting disease risk?” he continued. The method seeks to identify any likely disease-causing culprits in an “agnostic” manner, meaning that it combs through an onslaught of genetic information from patients with AAA, looking for commonalities. This, Snyder said, is the key to unraveling any number of genetic diseases.
* For More Information, Contact:
Marcelo Giarelli, MSN, RN, CCRN Ellen Fiss, Public Relations
Tampa General Hospital efiss@tgh.org
mgiarelli@tgh.org 813-844-6397
(813) 844-5001